|
9/24/2023 0 Comments Inferior pharyngeal constrictor7Ī recent study found that the swallowing-related severe late AE of lung infection significantly reduced the OS in NPC patients (adjusted Hazard Ratio 6.3, 95% CI 1.6–24.2, p=0.007). 7, 8 Together with other late AEs, these conditions impair quality of life in such patients. 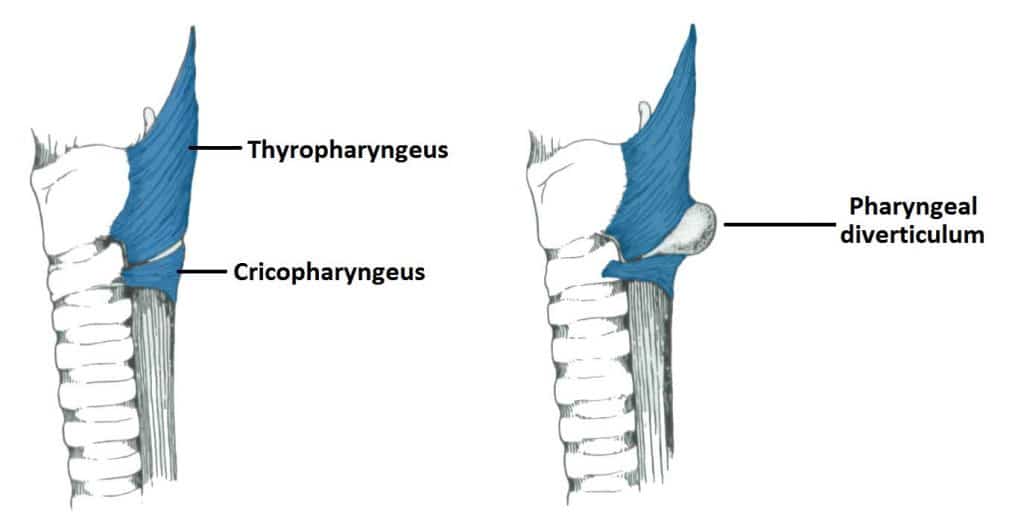
However, at long-term follow up, patients who received IMRT still suffer from many kinds of swallowing-related severe late AE such as malnutrition, dysphagia, xerostomia, trismus and aspiration pneumonia. Furthermore, IMRT could significantly reduce the incidence of the swallowing-related late adverse effects (AEs) of trismus and xerostomia, compared to 2D or 3D radiotherapy treatments (OR = 0.18 95% CI 0.04–0.83 p<0.05 OR = 0.18 95% CI 0.07–0.46 p<0.05, respectively). 3 Zhang et al 5 in a meta-analysis, found that IMRT treatment significantly improved both 5-year OS (Odds Ratio = 1.51 95% confidence interval 1.23–1.87 p<0.05) and local control (OR = 1.94 95% CI 1.53–2.46 p < 0.05). 
3–6 For example, the RTOG-0225 trial demonstrated that IMRT could be used in multi-institutional setting with 2-year progression-free and overall survival (OS) rates of 72.7% and 80.2%, respectively. 1 In addition to systemic chemotherapy, 2 numerous studies have confirmed the usefulness of intensity-modulated radiotherapy (IMRT). The results for treatment of nasopharyngeal carcinoma (NPC) have improved in recent decades. 
The mean doses of pharyngeal constrictor muscle (PCM), superior-middle PCM (SMPCM), and superior PCM (SPCM) were significantly higher in those with severe (≥G3) lung infection than in those without (65.7 vs 62.2 Gy, p = 0.036 68.1 vs 64.2 Gy, p = 0.015 and 70.0 vs 65.9 Gy, p = 0.012, respectively). This study enrolled 185 (43 female, 142 male) NPC patients, mean age 52.4 years, primarily with Stage III (93, 50.3%) or Stage IV (67, 36.2%) disease.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
